Fears for patient safety as extra beds crammed into Forth Valley Royal rooms
and live on Freeview channel 276
The demand for inpatient care has been so great in recent weeks that health chiefs have been forced to put two additional beds into rooms designed for four, as well as placing patients into treatment rooms and other contingency areas.
However, some staff say that patient safety is a “concern”.
Advertisement
Hide AdAdvertisement
Hide AdOne experienced nurse said: “It’s shocking what is happening.
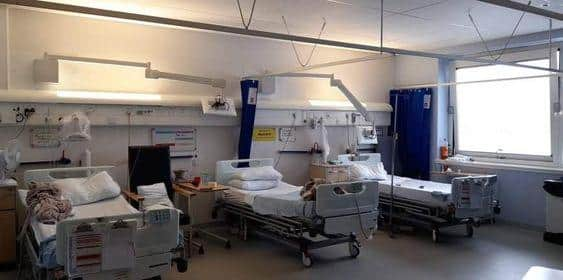

"Patients are getting no privacy in these rooms. They are designed for four people with four beds, chairs, curtains, and most importantly four oxygen portals and call buzzers.
“But now they are putting an additional two beds in some rooms.
"What if someone needs to use a commode? There’s no privacy at all.
Advertisement
Hide AdAdvertisement
Hide Ad"They are even giving the people in the extra beds door bells to call for staff.
"There’s also the worry that if there was a cardiac arrest whether with six patients and beds in a room there would be enough space to bring in the equipment needed to deal with the emergency.”
The nurse said that she also had concerns that the majority of the staff being employed were newly-qualified staff nurses and were not receiving the correct support, but instead were being “thrown in at the deep end”.
Health chiefs have admitted that at periods of “exceptionally high demand” they are being forced into these drastic measures.
Advertisement
Hide AdAdvertisement
Hide AdThey say that screens have been purchased to give people privacy but admit that call bells are being handed out for patients to request assistance.
It comes as NHS Forth Valley’s acute hospital recorded Scotland’s worst A&E waiting time figures since current records began.
Last week only 50.3 per cent of people who turned up at the Larbert hospital’s emergency department were seen within the four-hour target set by the Scottish Government.
Latest figures show 1162 people attended the A&E with 578 of them waiting over four hours, 149 over eight hours and 25 more than 12 hours.
Advertisement
Hide AdAdvertisement
Hide AdAcross Scotland, 71.3 per cent of patients were admitted, discharged or transferred within four hours of arriving at an A&E unit.
A spokeswoman for NHS Forth Valley said: “Forth Valley Royal Hospital, like many hospitals across Scotland, is exceptionally busy and we are seeing high numbers of seriously ill patients attending our Emergency Department and acute assessment units who require to be admitted to hospital for treatment.
“Due to pressures on local social care services, we also have a very high number of patients who are clinically well enough to leave hospital but are unable to do so due to delays in arranging care at home support and the availability of places in local care homes.
"However, despite these pressures, our staff continue to provide high quality care and are doing everything possible to meet the needs of local patients and their families at this very challenging time. Staffing numbers, skill mix and capacity are also closely monitored on a daily basis by a team of senior clinical and service leads to ensure the continued delivery of safe and effective care across the hospital site.”
Advertisement
Hide AdAdvertisement
Hide AdShe added: “As emergency situations can occur anywhere in the hospital, including patient bathrooms, our emergency equipment is mobile and can access all parts of our inpatient bays including areas used to care for an additional patient.”
In August, we told the story of one patient unhappy at being moved to three different wards in as many days, finally ending up in what she called a “cupboard” which was in fact a ward treatment room.
Iona Macaulay, 73, of Camelon said: "People are being moved about like pieces of furniture.”
"I can’t blame the staff, they were only doing their job, but it’s an absolutely shocking way to treat people who are sick.
Advertisement
Hide AdAdvertisement
Hide Ad"There’s serious problems in this hospital if they don’t have enough room for everyone who needs it.”
The health board added that it had taken steps to reduce pressure and create additional capacity across local health and care services.
This included opening additional beds and contingency areas in Forth Valley Royal Hospital, Falkirk Community Hospital and Bo’ness Community Hospital, adapting and expanding the use of the Day Surgery Unit and introducing new services to reduce pressure on the Emergency Department.
The Hospital at Home service has also relocated to a new base at Falkirk Community Hospital to enable it to support more people in their own homes who in the past would have been admitted to hospital for treatment.
Advertisement
Hide AdAdvertisement
Hide AdLocal politicians have promised to raise the issue of hospital pressures and patient care with the health board.
Michelle Thomson, Falkirk East MSP, said: "I treat any issues regarding patient safety with concern. I am raising the points outlined by the Falkirk Herald with NHS Forth Valley chief executive, Cathie Cowan.”
While Michael Matheson, Falkirk West MSP, said he was already in contact with the health board over the issue of improved care for patients with dementia and urged any constituents with concerns to contact his office.
Commenting on the issue of new staff, the NHS FV spokeswoman added: “Over the last few months, we have employed a number of newly-qualified and more experienced nurses. The majority of our newly-qualified nurses completed placements within Forth Valley Royal Hospital during their training and had therefore gained experience in many of the areas where they are now working in permanent posts. However, all newly qualified nurses undergo a detailed induction and are also supported by senior ward staff and our Practice Development Team and many maintain links with the mentors who supported them throughout their training.
Advertisement
Hide AdAdvertisement
Hide Ad“Additional senior nurse cover has been introduced to support staff during the overnight period and a two new Clinical Nurse Managers are currently being recruited to provide senior leadership and support across our Emergency Department and inpatient services.”